
(616) 846-3400
Fax: (616) 846-3406

(616) 846-3400
Fax: (616) 846-3406

 The medical condition that is referred to as poor circulation can be an indication of health issues that may exist in the body. It may be caused by poor dietary habits or sitting for extended periods of time. Additional causes may consist of diabetes, peripheral artery disease (PAD), or blood clots in the legs. Many patients experience symptoms that are indicative of poor circulation, and these may include a lack of energy, feet that are cold the majority of the time, or a tingling or numbing sensation in the hands and feet. Other symptoms may consist of having a poor memory, a weakened immune system, or a loss of appetite. Research has indicated that maintaining a healthy diet and engaging in an exercise regime may be helpful in treating poor circulation. It’s important to drink plenty of fresh water daily, in addition to avoiding alcohol. If poor circulation is affecting your feet, it is suggested to speak to a podiatrist who can properly diagnose and treat this condition.
The medical condition that is referred to as poor circulation can be an indication of health issues that may exist in the body. It may be caused by poor dietary habits or sitting for extended periods of time. Additional causes may consist of diabetes, peripheral artery disease (PAD), or blood clots in the legs. Many patients experience symptoms that are indicative of poor circulation, and these may include a lack of energy, feet that are cold the majority of the time, or a tingling or numbing sensation in the hands and feet. Other symptoms may consist of having a poor memory, a weakened immune system, or a loss of appetite. Research has indicated that maintaining a healthy diet and engaging in an exercise regime may be helpful in treating poor circulation. It’s important to drink plenty of fresh water daily, in addition to avoiding alcohol. If poor circulation is affecting your feet, it is suggested to speak to a podiatrist who can properly diagnose and treat this condition.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact Dr. Robbi Young of Grand Haven Foot & Ankle. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Poor blood circulation in the feet and legs is often caused by peripheral artery disease (PAD), which is usually the result of a buildup of plaque in the arteries. Plaque buildup, or atherosclerosis, can be the result of excess calcium and cholesterol in the bloodstream. This restricts how much blood can flow through arteries. Reduced blood flow to a certain area of the body severely limits the amount of oxygen and nutrients that part of the body receives. This leads to degeneration in the muscles and other tissues. Sometimes, poor blood circulation in the feet and legs can be caused by other conditions, such as the damaging or inflammation of blood vessels, known as vasculitis.
The lack of oxygen and nutrients caused by poor blood circulation can restrict muscle growth and development, as well as cause muscle pain and cramps, weakness, and stiffness. Other common symptoms include numbness in the legs and feet, skin discoloration in the affected limbs, slower nail and hair growth, and erectile dysfunction in men. In more severe cases of PAD, pain can be present even when a person isn't exercising, and may range from mildly uncomfortable to completely debilitating.
Poor blood circulation in the feet and legs is more common in those who are overweight or obese, have diabetes, high blood pressure, high cholesterol, who smoke, or who have a family history of PAD or related conditions such as a heart attack, stroke, etc. Diabetes and smoking place a person at greatest risk for developing poor blood circulation, although advanced age, over 50, can also increase risk.
If you are experiencing poor blood circulation in the feet and legs caused by PAD, it is important to make changes to your lifestyle in order to reduce your risk of experiencing a heart attack or stroke caused by this condition. If you smoke, quit completely. This will increase the amount of oxygen in your bloodstream. Exercising and reducing the saturated fats in your diet. Saturated fats come from fatty meats, fried foods, whole milk, etc., can make a difference in improving blood circulation in feet. It is also important to avoid developing influenza and to carefully control your blood sugar if you have diabetes.
Your doctor may recommend combining lifestyle changes with a prescription medication regimen to improve blood circulation. The most commonly-used medications for PAD are called statins and work by blocking the amount of enzymes in your body that produce cholesterol. They are known by the brand names Zocor, Lipitor, Crestor, and others.
 Sever’s disease is a painful heel condition that only affects children. Swelling of the growth plate is what causes this disease, along with discomfort and pain. Children that are involved in sports are more likely to have this affiliation, because injuries to the growth plate are caused by weight-bearing activities. Stretching can help to prevent Sever’s disease, and it can also assist in the healing process. Movements that stretch the hamstring, calf muscles, and tendons on the back of the leg should be performed 2 to 3 times a day, with the stretch being held for around 20 seconds. Even if there is only pain in one heel, the stretches should be done with both legs. Exercises that strengthen the muscles surrounding the shin will also help alleviate some discomfort and help to prevent this condition from developing again. If you think your child may have Sever’s Disease, then it is highly recommended to consult with a podiatrist in order to receive more information and proper treatment.
Sever’s disease is a painful heel condition that only affects children. Swelling of the growth plate is what causes this disease, along with discomfort and pain. Children that are involved in sports are more likely to have this affiliation, because injuries to the growth plate are caused by weight-bearing activities. Stretching can help to prevent Sever’s disease, and it can also assist in the healing process. Movements that stretch the hamstring, calf muscles, and tendons on the back of the leg should be performed 2 to 3 times a day, with the stretch being held for around 20 seconds. Even if there is only pain in one heel, the stretches should be done with both legs. Exercises that strengthen the muscles surrounding the shin will also help alleviate some discomfort and help to prevent this condition from developing again. If you think your child may have Sever’s Disease, then it is highly recommended to consult with a podiatrist in order to receive more information and proper treatment.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Sever's disease, also known as calcaneal apophysitis, is a medical condition that causes heel pain in children’s feet while they’re growing. Sever's disease occurs most commonly in boys and girls between the ages of 8 and 14.
Sever's disease occurs when the child’s growth plate, or the calcaneal epiphysis, an area attached to the Achilles tendon, is injured or when the muscles and tendons of the growing foot do not keep pace with bone growth. The result is constant pain experienced at the back of the heel and the inability to put any weight on the heel. This forces the child to bear weight on their toes while walking. When a toe gait develops, the child must change the way they walk to avoid placing weight on the painful heel. If this is not properly addressed, this can lead to further developmental problems.
The most common symptom of Sever's disease is acute pain felt in the heel when a child engages in physical activity such as walking, jumping or running. Children who are active athletes are among the group most susceptible to experiencing Sever's disease. This is due to the extreme stress and tension placed on their growing feet. The rolling movement of the foot during walking or running and obesity are both additional conditions linked to causing Sever's disease.
The first step in treating Sever's disease is to rest the foot and leg and avoid physical activity. Over the counter pain-relieving and anti-inflammatory medications can be helpful for reducing the amount of heel pain. A child with Sever's disease should also wear shoes that properly support the heel and the arch of the foot. Consider purchasing orthotic shoe inserts which can help support the heel and foot while it is healing. Most patients with Sever's disease symptoms report an eventual elimination of heel pain after wearing orthotic insoles that support the affected heel.
Sever's disease may affect either one heel or both. It is important for a child experiencing heel pain to be examined by a foot doctor who can apply the squeeze test. The squeeze test compresses both sides of the heel in order to determine if there is intense pain. Discourage any child diagnosed with Sever's disease from going barefoot as this can intensify the problem. Apply ice packs to the affected painful heel two or three times a day for pain relief.
Exercises that help stretch the calf muscles and hamstrings are effective at treating Sever's disease. An exercise known as foot curling has also proven to be very effective at treating Sever's disease. When foot curling, the foot is pointed away from the body, then curled toward the body to help stretch the muscles. The curling exercise should be done in sets of 10 or 20 repetitions and repeated several times throughout the day.
Treatment methods can continue for at least 2 weeks and as long as 2 months before the heel pain completely disappears. A child can continue doing daily stretching exercises for the legs and feet to prevent Sever’s disease from returning.
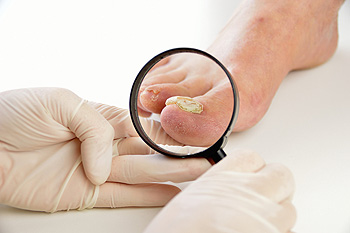 If you notice the color of your toenail becoming white or yellow, you may have what is referred to as toenail fungus. It is the result of an infection that is caused by a fungus, and the first noticeable symptoms may be discoloration of the toenail. The nail may appear darker as the infection spreads, in addition to the texture becoming compromised. This may become apparent if the nail should begin to crumble which may cause the toenail to separate from the nail bed. This type of fungus lives and thrives in moist and warm environments, which may include shoes that are not made with breathable materials. Additionally, showers and surrounding areas, locker rooms, or public pools may be a breeding ground for this type of fungus to live, and it is advised to wear appropriate shoes while in these areas. It may be beneficial to wash and dry the feet frequently, change socks and shoes daily, and properly trim the toenails. If you are afflicted with toenail fungus, it is suggested to seek the counsel of a podiatrist who can properly treat this condition.
If you notice the color of your toenail becoming white or yellow, you may have what is referred to as toenail fungus. It is the result of an infection that is caused by a fungus, and the first noticeable symptoms may be discoloration of the toenail. The nail may appear darker as the infection spreads, in addition to the texture becoming compromised. This may become apparent if the nail should begin to crumble which may cause the toenail to separate from the nail bed. This type of fungus lives and thrives in moist and warm environments, which may include shoes that are not made with breathable materials. Additionally, showers and surrounding areas, locker rooms, or public pools may be a breeding ground for this type of fungus to live, and it is advised to wear appropriate shoes while in these areas. It may be beneficial to wash and dry the feet frequently, change socks and shoes daily, and properly trim the toenails. If you are afflicted with toenail fungus, it is suggested to seek the counsel of a podiatrist who can properly treat this condition.
For more information about treatment, contact Dr. Robbi Young of Grand Haven Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Toenail fungus is a frustrating problem that affects many people. It can be persistent and hard to get rid of. As many different types of fungi are present throughout the environment, it is very easy to contract toenail fungus.
The feet are especially susceptible to toenail fungus because shoes and socks create the ideal dark and moist environment that fungal infections thrive in. While fungal infections of the nail plate are quite common, if left untreated they can spread beyond the toenail and into the skin and other parts of the body.
Signs of toenail fungus include a thickened nail that has become yellow or brown in color, a foul smell, and debris beneath the nail. The toe may become painful due to the pressure of a thicker nail or the buildup of debris.
Treatment for toenail fungus is most effective during the early stages of an infection. If there is an accumulation of debris beneath the nail plate, an ingrown nail or a more serious infection can occur. While each treatment varies between patients, your podiatrist may prescribe you oral medications, topical liquids and creams, or laser therapy. To determine the best treatment process for you, be sure to visit your podiatrist at the first signs of toenail fungus.
Morton's Neuroma, also called Intermetatarsal Neuroma or Plantar Neuroma, is a condition that affects the nerves of the feet, usually the area between the third and fourth toe. Neuroma refers to a benign growth that can occur in different parts of the body. Morton's Neuroma strictly affects the feet. This condition causes the tissue around the nerves that lead to the toes becoming thick, causing pain in the ball of the foot.
This condition can be caused by injury, pressure or irritation. Normally no lump will be felt, but instead burning pain in the ball of the foot will be experienced. Numbness and tingling may also occur. With the onset of this condition, a person may feel pain when tight or narrow shoes are worn. As the condition worsens, the pain may persist for days, or even weeks.
Persistent foot pain should always be a concern. The foot should be examined by a podiatrist if pain persists longer than a few days with no relief from changing shoes. The earlier the foot is examined and treated, the less chance there will be for surgical treatment.
There are some factors that can play a role in the development of Morton's Neuroma. These include wearing ill-fitting shoes that cause pressure to the toes, such as high heels. Also, high impact exercise may contribute to the cause of this condition. Morton’s Neuroma may also develop if the foot sustains an injury. Another cause includes walking abnormally due to bunions or flat feet. This causes excessive pressure and irritates the tissue. At times, people are affected for no determinable reason.
Podiatrists can alleviate the effects of this condition using a treatment plan to help decrease the pain and heal the foot tissue. Depending upon the severity of the Morton's Neuroma, the treatment plan can vary. For cases that are mild to moderate, treatments may include applying padding to the arch to relieve pressure from the nerve and reduce compression while walking. Ice packs can also help reduce swelling. The podiatrist may also create a custom orthotic device to support the foot and reduce compression and pressure on the affected nerve. The doctor will probably advise against partaking in activities that cause constant pressure on the affected area. They may provide wider shoes to ease the pressure from the toes. If these treatments do not relieve the symptoms of this condition, the doctor may use injection therapy.
Surgical treatment may be recommended by the podiatrist if all other treatments fail to provide relief. Normally, the podiatric surgeon will decide on either a surgical procedure that involves removal of the affected nerve or will choose surgery to release the nerve. After examination, the surgeon will decide on the best approach to treat the problem.
Recovery varies according to the type of surgical procedure. The patient will also be instructed on the best shoe wear to prevent the return of this condition, along with changes to workout routines, if this was a cause. Preventative measures are important in ensuring the condition does not return.
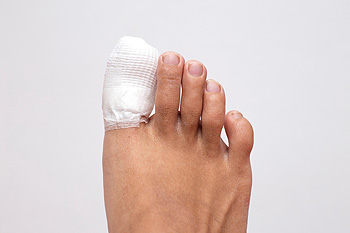 Everyone stubs their toe from time to time, but sometimes stubbing it too hard can result in a broken toe. Stubbing your toe causes immediate pain, but it usually only takes a couple minutes to subside. If the pain does not dissipate and continues for a long time after the initial blow, you may be dealing with a broken bone. Some signs of a broken toe are swelling, discoloration, and bruising. If you put weight on your foot and become unable to walk due to pain, your toe may be broken. If you suspect that your toe is broken, the best idea is to seek help from a medical professional. A doctor will most likely use an x-ray to determine whether your toe is broken and how to properly treat it. If you think you may have a broken toe or want additional information, then you should consult a podiatrist for help.
Everyone stubs their toe from time to time, but sometimes stubbing it too hard can result in a broken toe. Stubbing your toe causes immediate pain, but it usually only takes a couple minutes to subside. If the pain does not dissipate and continues for a long time after the initial blow, you may be dealing with a broken bone. Some signs of a broken toe are swelling, discoloration, and bruising. If you put weight on your foot and become unable to walk due to pain, your toe may be broken. If you suspect that your toe is broken, the best idea is to seek help from a medical professional. A doctor will most likely use an x-ray to determine whether your toe is broken and how to properly treat it. If you think you may have a broken toe or want additional information, then you should consult a podiatrist for help.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The forefoot is composed of five metatarsal bones and fourteen phalanges. Each toe has three phalanges except for the big toe which only has two. Our toes play an essential role to the walking process, which is why a broken toe could seriously disrupt one’s ability to move around. Toe fractures are common and can be very painful. Fortunately, these injuries rarely require surgery and usually heal with rest and a change in activity.
Broken toes typically result from a traumatic event such as falling, stubbing the toe, or dropping something on the toe. Traumatic toe fractures may be categorized as either minor or severe fractures. At times, one may hear a “pop” or “crack” sound when the bone breaks. Common symptoms of a traumatic toe fracture include pain, throbbing, bruising, swelling, and redness.
Another type of toe fractures is a stress fracture. These injuries usually appear in the form of small hairline breaks on the bone. Stress fractures develop after repetitive activity instead of a single injury. Stress fractures occur when the muscles in the bone become too weak to absorb impact. Consequently, the toe bone becomes vulnerable to any pressure and impact it endures. Symptoms for a stress fracture in the toe include swelling without bruising, tenderness to the touch, pain that goes away with rest, and pain after walking or running.
If you suspect that you have a broken toe, you should make an appointment with your podiatrist. He or she will likely diagnose you by performing a physical exam and an X-ray. Treatment for a broken toe may include the R.I.C.E. method, buddy taping, surgery, or antibiotics. The R.I.C.E. method (Rest, Ice, Compression, and Elevation) is a common treatment method for many injuries because it decreases pain. Buddy tapping involves wrapping the injured toe next to an adjacent toe to keep it supported and protected. These two methods have proven to be effective in the healing process for toe fractures. The estimated healing time for a broken toe is approximately four to six weeks. If the injury becomes infected or requires surgery, the estimated healing time may take eight weeks or more.