
(616) 846-3400
Fax: (616) 846-3406

(616) 846-3400
Fax: (616) 846-3406
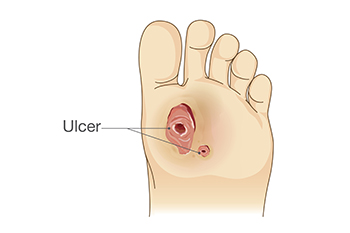
Non-healing foot ulcers in diabetic patients are influenced by a myriad of factors, including the wound environment, the patient's general health, and the medications they are taking. A compromised wound environment, often characterized by high bacterial load, excess moisture, or inadequate blood supply due to peripheral arterial disease, can impede healing. Additionally, the patient's overall health status plays a significant role, with conditions like obesity, smoking, and immune system deficiencies hindering the body's ability to repair tissues. Medications such as corticosteroids and certain chemotherapeutic agents may also interfere with wound healing processes. Addressing these multifaceted challenges requires a comprehensive approach, encompassing wound debridement, infection control, and optimizing the patient's general health through lifestyle modifications and medication adjustments. If you suffer from diabetic foot ulcers, it is strongly suggested that you are under a podiatrist to enhance healing outcomes and reduce the risk of serious complications.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
 Diabetic foot ulcers are a serious concern for people with diabetes, as they can lead to severe complications. These ulcers form due to a combination of poor circulation, nerve damage, and impaired wound-healing capabilities, all common in diabetics. To lower the risk of complications, it's important to manage blood sugar levels diligently, as high glucose can further impair healing. Regular inspections of the feet for any cuts, bruises, or changes are essential to catch problems early. Making regular appointments with a podiatrist, or foot doctor, can help with this process. Wearing properly fitting shoes and avoiding walking barefoot can also prevent injuries. If an ulcer does develop, it is important to seek immediate medical attention to treat the wound and any infections. Maintaining cleanliness, applying appropriate dressings, and possibly using antibiotics are typical steps in managing foot ulcers. If you are diabetic and at risk for developing foot ulcers, it is suggested that you add a podiatrist to your care team.
Diabetic foot ulcers are a serious concern for people with diabetes, as they can lead to severe complications. These ulcers form due to a combination of poor circulation, nerve damage, and impaired wound-healing capabilities, all common in diabetics. To lower the risk of complications, it's important to manage blood sugar levels diligently, as high glucose can further impair healing. Regular inspections of the feet for any cuts, bruises, or changes are essential to catch problems early. Making regular appointments with a podiatrist, or foot doctor, can help with this process. Wearing properly fitting shoes and avoiding walking barefoot can also prevent injuries. If an ulcer does develop, it is important to seek immediate medical attention to treat the wound and any infections. Maintaining cleanliness, applying appropriate dressings, and possibly using antibiotics are typical steps in managing foot ulcers. If you are diabetic and at risk for developing foot ulcers, it is suggested that you add a podiatrist to your care team.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Athlete's foot, known medically as tinea pedis, is a common fungal infection that affects the skin of the feet. It thrives in warm, moist environments, such as locker rooms, swimming pools, and communal showers. This condition is caused by various types of fungi, primarily belonging to the dermatophyte group. Symptoms of athlete's foot include itching, burning, and stinging sensations, frequently between the toes or on the soles of the feet. As the infection progresses, the skin may become red, cracked, and blistered. In severe cases, it can lead to the development of painful ulcers or secondary bacterial infections. Athlete's foot is extremely contagious and can spread through direct contact with infected surfaces or by sharing contaminated items like towels or shoes. Practicing good foot hygiene, wearing breathable footwear, and keeping feet dry can help prevent the occurrence of this bothersome condition. If you have developed this ailment, it is suggested that you visit a podiatrist who will often prescribe medication for relief and healing.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
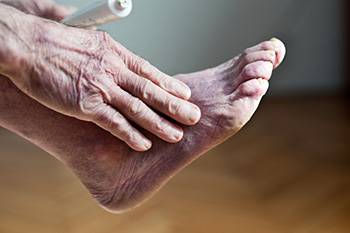
Poor foot circulation can silently wreak havoc on your health, manifesting in various troubling symptoms. One of the most common indicators is cold feet, often accompanied by numbness or tingling sensations. Swelling in the feet and ankles, particularly after prolonged periods of sitting or standing, may also signify compromised circulation. Additionally, you may notice changes in skin color, with the feet appearing pale or bluish. These symptoms can interfere with daily activities and diminish your quality of life. Several factors contribute to poor foot circulation, including underlying health conditions such as peripheral artery disease, diabetes, or hypertension. Lifestyle choices, like smoking, a sedentary lifestyle, and a diet high in saturated fats, can worsen poor circulation. Furthermore, obesity and certain medications may also impair circulation. If you are experiencing any of the above symptoms, it is suggested that you are under the care of a podiatrist who can help you to manage this condition.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact Dr. Robbi Young of Grand Haven Foot & Ankle. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.